Mitral Valve
2D
Inspect leaflets.
- Thickened / calcified. Leaflet thickness should be <5mm.
- Excess movement.
- Restricted movement.
PSAX - A1-3 and P1-3. Measure with planimetry if good view. Valve area 4-6cm2.
A4C - A2/3 by septum and P1 laterally.
A2C - P1/3 either side and A2 in middle.
A3C - A2 and P2 (like PLAX).
MV prolapse if any part of either leaflet >2mm behind annulus in PLAX or coaptation point of leaflets behind annulus in A4C.
Papillary muscles are anterolateral and postero-medial (infero-septal wall).
Myxomatous degeneration - thickened annulus/leaflets with excessive movement.
Rheumatic - leaflet tip thickening with restricted movement.
Mitral Stenosis
CW and PW
CW of forward flow
Measuring peak velocity (E) will give the pressure gradient across the valve but values for this not part of BSE grading.
PHT by measuring downward slope of E wave. Gets longer with severity.
Valve area of 1cm2 has a PHT of 220ms therefore:
MV area = 220/PHT
Trace MV inflow to get VTI and mean pressure gradient.
Can use continuity equation for valve area (volume of blood entering LV = volume leaving).
Measure LVOT (to calculate CSA), VTI of LVOT with PW and VTI of MV inflow with PW.
CSAA x VTIA = CSAM x VTIM
or
CSAM = SVA/VTIM
AR will shorten PHT thus underestimating severity.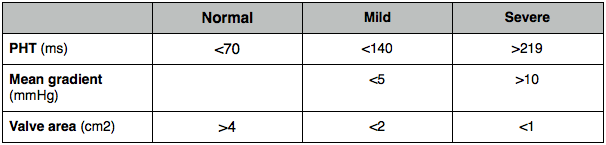
Mitral regurgitation
MR functional if valve structure normal but other pathology causing it eg dilated LV (can be of any severity).
Colour
Trace jet area and LA area.
Note direction of jet - central, anterior, posterior. Eccentric jets usually away from abnormal leaflet. Central jets appear more severe than they are (entrainment - Venturi) and eccentric less severe.
Measure VC in PLAX or A4/3C (not A2C). Nyquist limit setting of 50-60.
CW and PW
CW will show density of jet.
PW 1cm into pulm vein (corner of LA next to septum and A4C).
Regurgitant volume
Measure MV annulus diameter in A4C and PW VTI at same point (i.e. the annulus not leaflet tips).
RV = SVMV - SVLVOT
RF = RV / SVMV x 100
ROA = RV / VTIMR
PISA (proximal isovelocity surface area) You’re a ninja at echo when you can do PISA
Blood flowing towards an orifice forms hemispheric shells which get smaller and faster as they approach the orifice.
The aliasing velocity (the bottom blue velocity) can be adjusted to match the velocity of blood in the shells at which point there will be a blue/red interface. At this position the aliasing velocity = the blood velocity. Reducing the velocity will make the shell bigger.
A4C - narrow width and minimise depth before zooming on MV.
Reduce aliasing velocity until clear hemisphere with red/blue interface seen on ventricular side.
Measure radius of hemisphere by measuring from edge to centre of valve leaflet orifice and then calculate its area:
PISA = 2 π r2
Flow = Area x Velocity
and continuity expresses that flowA = flowB so
Regurg flow rate = PISA x aliasing velocity
so
ROA x VmaxMR = PISA x aliasing velocity
or
ROA = PISA x aliasing velocity / Vmax MR
or
ROA = RFR / VmaxMR
Note this is at one instant so is velocity per second rather than for one whole cardiac cycle which is why VTI not used - I think would be more accurate if VTI used.